Using Silent Hypoxia In AI Algorithms As A Prognostic Indicator Of Cardiovascular Disease
Author: Amina Khalpey, PhD, Parker Wilson, BS, Brynne Rozell, BS, Zain Khalpey, MD, PhD, FACS
Silent hypoxia refers to a condition in which the peripheral tissues of the body are not receiving adequate oxygenation, while no obvious symptoms, like dyspnea or fatigue, are apparent. While this condition is often associated with chronic lung disease or obstructive sleep apnea (OSA), it is becoming increasingly clear that silent hypoxia may also serve as a biomarker for cardiovascular disease (CVD) and could be useful in predicting the onset and severity of CVD. Utilizing the presence of biomarkers like this, scientists can program AI algorithms to help predict CVD, resulting in earlier treatment and improved patient outcomes.
Cardiovascular Disease
CVD is a major health problem worldwide, accounting for over 17 million deaths each year. One of the major underlying mechanisms of CVD is the buildup of cholesterol plaques in the arteries, leading to restricted blood flow and oxygen delivery to the heart and other vital organs. As a result, the body may not receive enough oxygen to meet its needs, leading to silent hypoxia.
Studies have shown that silent hypoxia is associated with several risk factors for CVD, including age, obesity, smoking, and poor physical activity. In addition, individuals with silent hypoxia are also more likely to have high blood pressure, high cholesterol, and other predictors of poor cardiovascular health. These findings suggest that silent hypoxia may be a useful biomarker for predicting the onset of CVD, allowing for early intervention and prevention.
Advantages
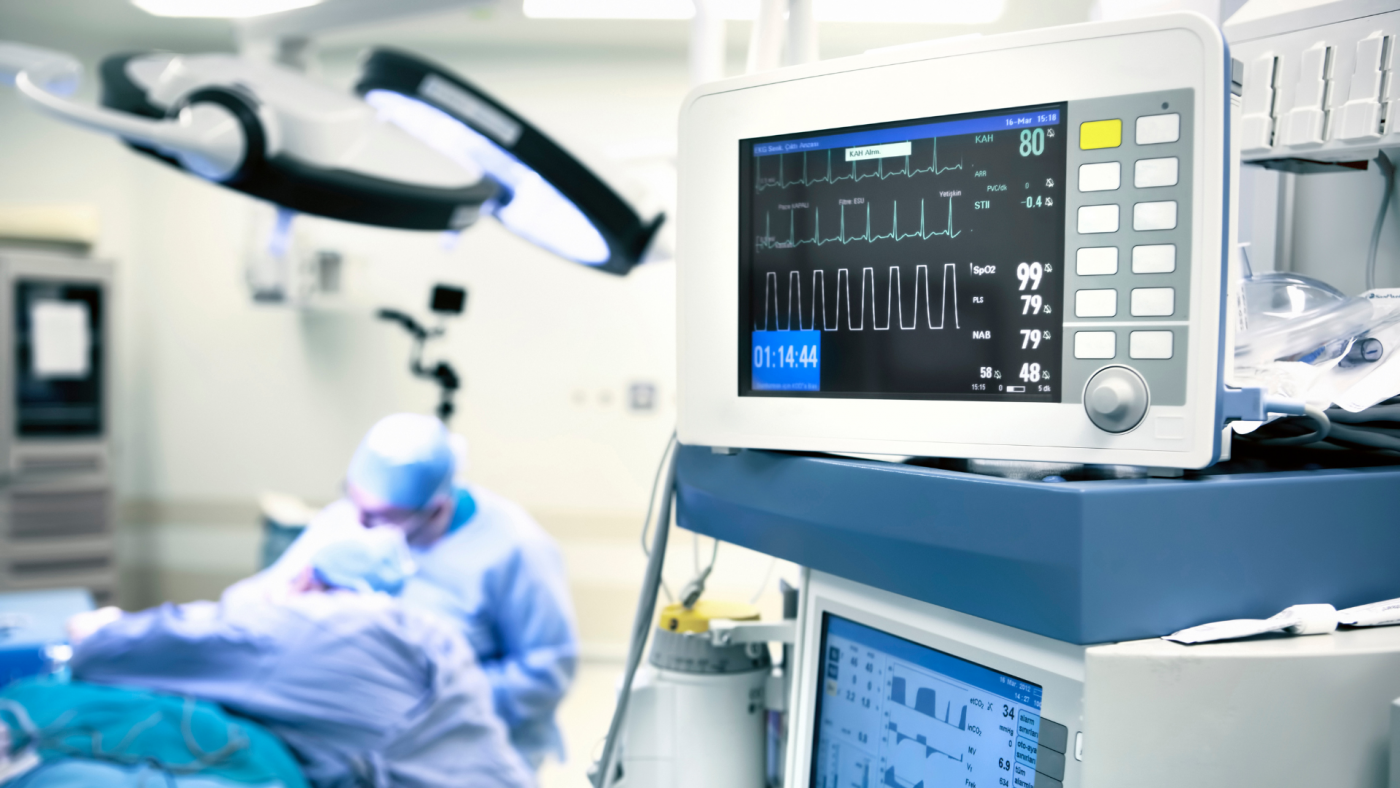
One of the key advantages of using silent hypoxia as a biomarker for CVD is its ease of measurement. Unlike traditional biomarkers, such as cholesterol levels or stress testing, silent hypoxia can be measured non-invasively using pulse oximetry. This simple and inexpensive metric involves attaching a small device to the fingertip that measures the oxygen saturation in the blood by measuring light absorption which is an indication of oxygenation. By measuring the amount of oxygen in the blood, healthcare professionals can quickly and easily determine whether an individual is suffering from silent hypoxia, and prognosticate on whether they are at increased risk for CVD.
Another advantage of using silent hypoxia as a biomarker for CVD is that it provides a more comprehensive picture of cardiovascular health. Unlike other markers that may only reflect one aspect of cardiovascular health, silent hypoxia reflects the overall oxygen delivery to the body. This information can be used to inform the development of targeted therapies and interventions, leading to better outcomes for individuals with CVD.
Algorithms and Silent Hypoxia
Silent hypoxia along with other vital signs and lab work can be comprehensively assessed by machine learning algorithms built to predict CVD. Algorithms devised by Khalpey AI Lab have already used silent hypoxia as a predictor of COVID-19 infection with remarkable sensitivity (Khalpey et al 2021). Given this success, it makes reasonable sense that silent hypoxia could be used alongside existing biomarkers and algorithms, like ASCVD, to provide earlier predictive power for CVD allowing for better longitudinal care of patients.
Inserting Silent Hypoxia Into AI Algorithms
In conclusion, silent hypoxia has the potential to be an important biomarker for cardiovascular disease. By providing a non-invasive, easy-to-measure, and comprehensive picture of cardiovascular health, silent hypoxia has the potential to improve the diagnosis and treatment of CVD. This could be especially powerful when combined with existing data into a algorithms that can better predict CVD. While further research is needed to fully develop the links between silent hypoxia, AI and CVD, the evidence to date suggests that it has the potential to play a significant role in improving cardiovascular health outcomes.
Bibliography
Khalpey ZI, Khalpey A, Modi B, Deckwa JL. Silent Hypoxia in Covid-19: A Machine Learning Algorithm for Early Prediction. J Am Coll Surg. 2021 Nov;233(5):e191.



